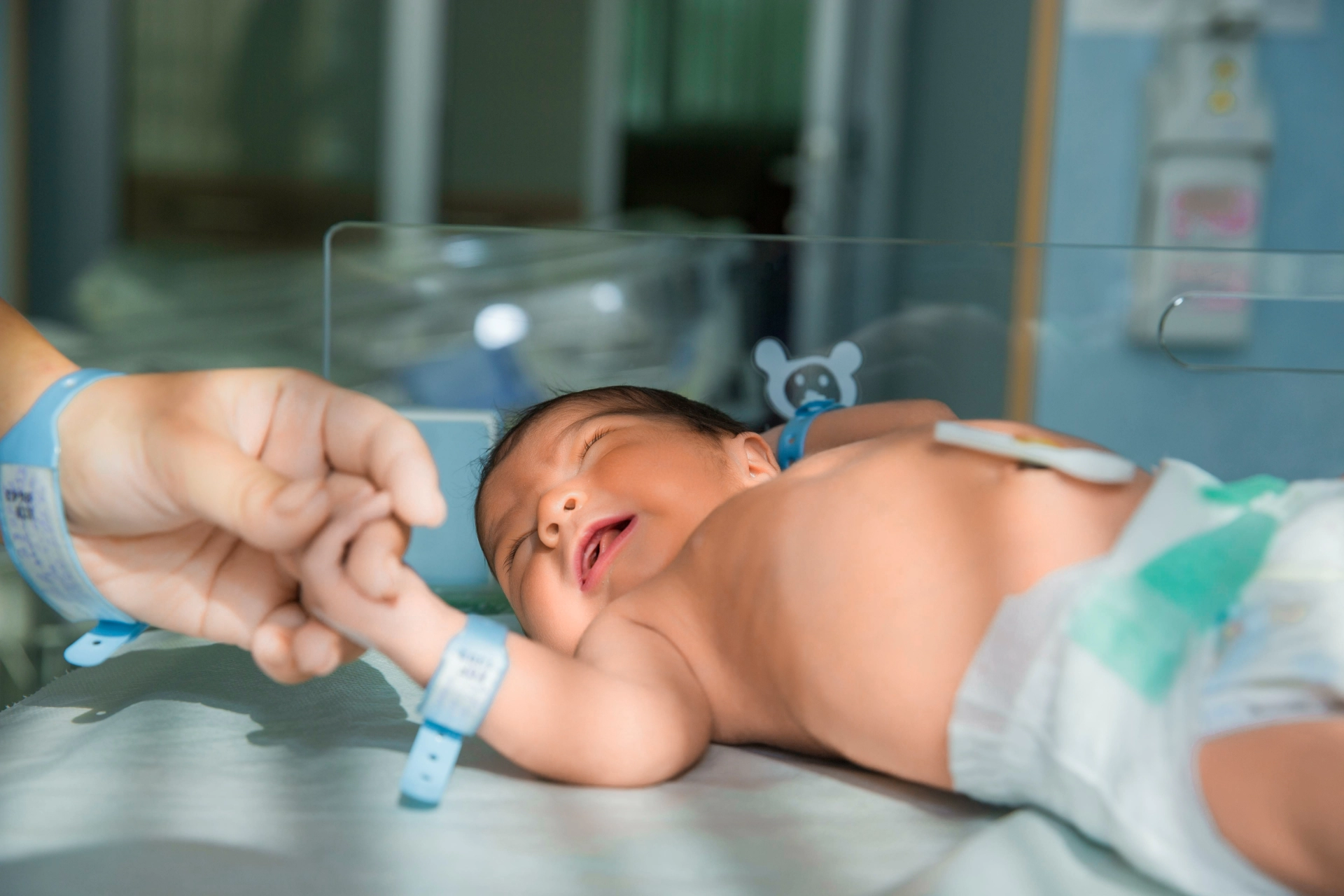
It’s one of the first things new parents might notice after birth — a yellowish tint to their baby’s skin or eyes. This condition, known as jaundice, is extremely common in newborns. In fact, it affects up to 60% of full-term babies and as many as 80% of preterm infants in the first week of life.
While it’s usually harmless and temporary, understanding why jaundice happens — and when it might signal a more serious issue — is important for every parent.
What Is Jaundice and Why Does It Happen?
Jaundice in newborns occurs when there’s too much bilirubin in the baby’s blood — a condition called hyperbilirubinemia. Bilirubin is a yellow pigment produced during the normal breakdown of red blood cells.
Before birth, the mother's liver does all the work of removing bilirubin for the baby. But after birth, that job shifts to the baby’s own liver — which may not be fully developed yet. If the liver can’t filter out bilirubin quickly enough, the substance starts to build up in the baby’s body, giving their skin and eyes a yellow hue.
This yellowing typically starts on the face and can spread to the chest, abdomen, arms, and legs as bilirubin levels rise. It’s easiest to spot in natural light, and in babies with darker skin, it may be more noticeable in the whites of the eyes or under the tongue.
Types of Newborn Jaundice
Not all jaundice is the same. There are several types, each with different causes and timeframes:
1.
Physiological Jaundice
. This is the most common type and occurs in nearly all newborns to some extent. It usually appears within 2 to 3 days after birth and disappears on its own within one to two weeks. It’s a natural part of the baby’s adjustment to life outside the womb as their liver matures.2.
Breastfeeding Jaundice
. This can develop in the first week of life when a baby isn’t getting enough breast milk. It may be due to difficulties with latching, a delay in milk coming in, or infrequent feedings. Less feeding means fewer bowel movements — and that leads to slower elimination of bilirubin from the body.3.
Breast Milk Jaundice
. This is different from breastfeeding jaundice. It typically appears after the first week and can last for a month or longer. In this case, certain substances in the mother's milk may interfere with how the baby’s liver processes bilirubin. Although it sounds concerning, breast milk jaundice is usually harmless and doesn’t require stopping breastfeeding.4.
Jaundice from Medical Conditions
. In some rare cases, jaundice can be caused by underlying health problems, such as:•Blood type incompatibility between mother and baby
•Bruising during birth (which increases red blood cell breakdown)
•Infections like sepsis
•Liver conditions, including biliary atresia
•Low oxygen levels at birth
•An excess of red blood cells
These forms of jaundice are less common but more serious and require immediate medical attention.
Symptoms to Watch For
The most obvious sign is yellowing of the skin and eyes. But parents should also monitor for other warning signs that may indicate severe jaundice or related complications:
•Bright yellow or orange-tinted skin
•Excessive sleepiness or trouble waking for feeds
•Baby is very fussy or difficult to calm
•Poor feeding, whether at the breast or with a bottle
•Not enough wet or dirty diapers
If jaundice seems to be getting worse after the first few days — or lasts longer than two weeks — it’s time to call your pediatrician.
How Is Jaundice Treated?
In most cases, no treatment is needed. As your baby’s liver matures and they begin feeding regularly, bilirubin levels naturally decrease. Frequent feedings — around 10 to 12 times a day — help stimulate more bowel movements, which remove bilirubin through the stool.
However, if bilirubin levels are too high or rising quickly, your baby’s doctor may recommend phototherapy — a safe and effective treatment that uses special blue lights to help break down bilirubin in the skin.
In rare, severe cases, where phototherapy isn’t enough, a treatment called an exchange transfusion may be necessary. This involves replacing a portion of the baby’s blood with donor blood to quickly reduce bilirubin levels. Fortunately, this is rarely needed with early monitoring and intervention.
While jaundice in newborns can be unsettling for new parents, it’s important to know that it’s usually a normal part of development. Most cases resolve without complications, especially when babies are well-fed and monitored closely.
Still, severe jaundice can pose serious risks, including brain damage if left untreated — so staying informed and knowing when to call your healthcare provider is essential.