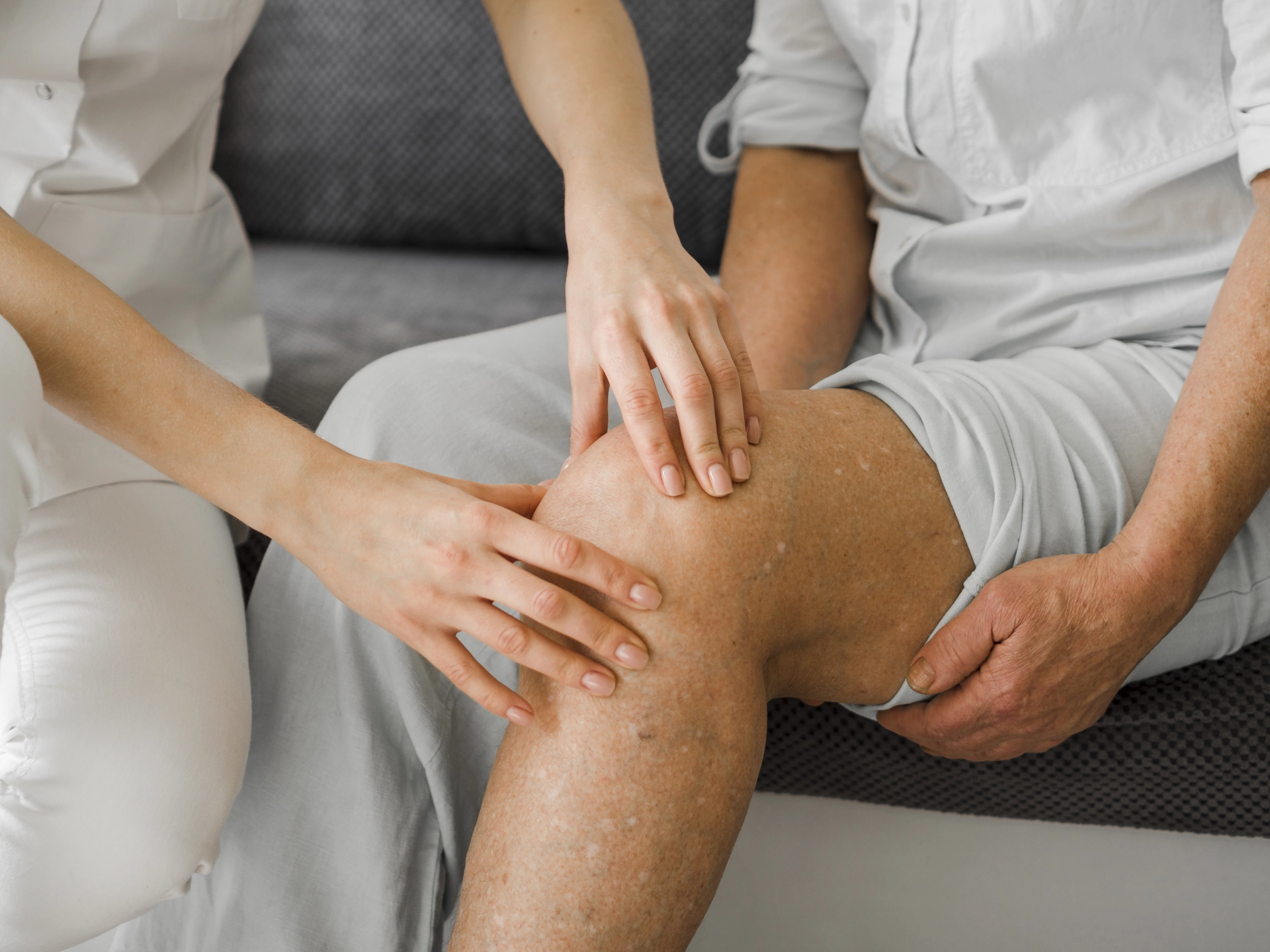
The knee joint is subjected to heavy daily stress. It is a fairly large joint, surrounded inside and outside by ligaments and tendons that ensure its stability. In fact, the articular cartilage itself has no nerve supply. With age, as cartilage wears down and body weight increases, the strain on the ligamentous apparatus also increases, leading to inflammation and destructive joint processes. At this stage, the patient feels pain in the knee joint.
According to global statistics, every 10th person over the age of 55 suffers from gonarthritis, and one in four of them becomes disabled and requires knee joint endoprosthesis surgery.
Causes of knee pain:
• Osteoarthritis, mainly caused by cartilage wear,
• Arthritis or joint inflammation, which can occur in rheumatoid arthritis, reactive arthritis, psoriatic arthritis, septic or infectious arthritis, periodic disease, gout, and other inflammatory joint conditions,
• Excess weight or obesity, which increases the load on the knees,
• Vitamin D deficiency,
• Impaired blood circulation in the lower limbs, for example due to varicose veins, pronounced lymphostasis, or obliterating arterial diseases of the legs,
• Certain types of anemia,
• Excessive physical exertion.
When to see a doctor:
• if the pain is persistent and gradually worsening, with only temporary relief from painkillers,
• if there is redness and localized warmth,
• if movement in the knees becomes difficult, especially when climbing up or down stairs,
• if a cracking or grinding sound (known as crepitus) is heard or felt in the knees,
• if there has been a wound or insect bite on the skin over the knee, followed by inflammation with redness and warmth.
Patients with gonarthritis (inflammation of the knee joint) may also have anemia. This may be a manifestation of the main disease or, in some cases, anemia itself may provoke joint inflammation. For example, in rheumatoid arthritis, blood tests may show anemia, thrombocytosis, and elevated ESR — indicators of disease activity. In such cases, it is not necessary to treat anemia with iron supplements; rather, proper anti-inflammatory therapy to control disease activity and flare-ups is sufficient, and laboratory markers will normalize on their own.
Anemia during inflammatory joint diseases may also be caused by prolonged use of nonsteroidal anti-inflammatory drugs (NSAIDs) such as diclofenac, ibuprofen, aertal, or indomethacin, which can lead to gastritis or peptic ulcers. One possible manifestation of these complications is anemia.
Knee pain can also be occupational. For example, knee injuries are very common among football players, since football involves fast running, sudden stops and turns, jumping, and kicking. Players may stretch or tear cruciate ligaments, damage the menisci, dislocate the kneecap, or develop inflammation or muscle strain.
A deficiency of vitamin D and magnesium can also cause knee and muscle pain. It is particularly important to replenish magnesium deficiency, as all enzymes involved in vitamin D metabolism require magnesium as a cofactor. Even when magnesium levels in bone tissue decrease, its concentration in the blood may remain within the normal range — this is known as chronic latent magnesium deficiency.