Breast cancer is influenced by many factors. Some—such as genetics, age, and family history—cannot be changed. However, research shows that healthy lifestyle choices combined with regular screenings can significantly lower risk and improve early detection.
Although prevention cannot be guaranteed, proactive steps can reduce your chances of developing breast cancer and increase the likelihood of detecting it early, when treatment is most effective.
1. Maintain a healthy weight
Excess weight, especially after menopause, increases risk because fat tissue produces estrogen. Maintain a stable, healthy weight through balanced nutrition and regular activity.
2. Stay physically active
Exercise helps regulate hormones and control weight. Aim for 150 minutes of moderate activity or 75 minutes of vigorous exercise weekly, plus strength training twice a week.
3. Limit alcohol
Alcohol increases breast cancer risk. If you drink, limit it to one drink per day—or avoid it entirely.
4. Choose a balanced diet
There is no single “anti-cancer diet,” but eating fruits, vegetables, whole grains, legumes, and healthy fats supports overall health. Reduce processed meat, red meat, sugary drinks, and heavily processed foods.
5. Avoid smoking
Smoking is linked to many cancers, including breast cancer. Quitting greatly benefits overall health.
6. Breastfeed if possible
Breastfeeding may slightly reduce risk, especially when continued longer.
7. Use hormones carefully
Hormone replacement therapy and some hormonal contraceptives may slightly increase risk. Always discuss options with your doctor and use the lowest effective dose for the shortest time.
8. Know your family history
Understand cancer history on both sides of your family.
9. Take extra steps if high-risk
High-risk individuals may need earlier screening, preventive medications, genetic counseling, or other preventive strategies.
10. Prioritize regular screening
Healthy habits reduce risk—but screening saves lives. Early detection greatly improves outcomes. Screening may include:
• Clinical breast exams
• Mammography based on age and risk
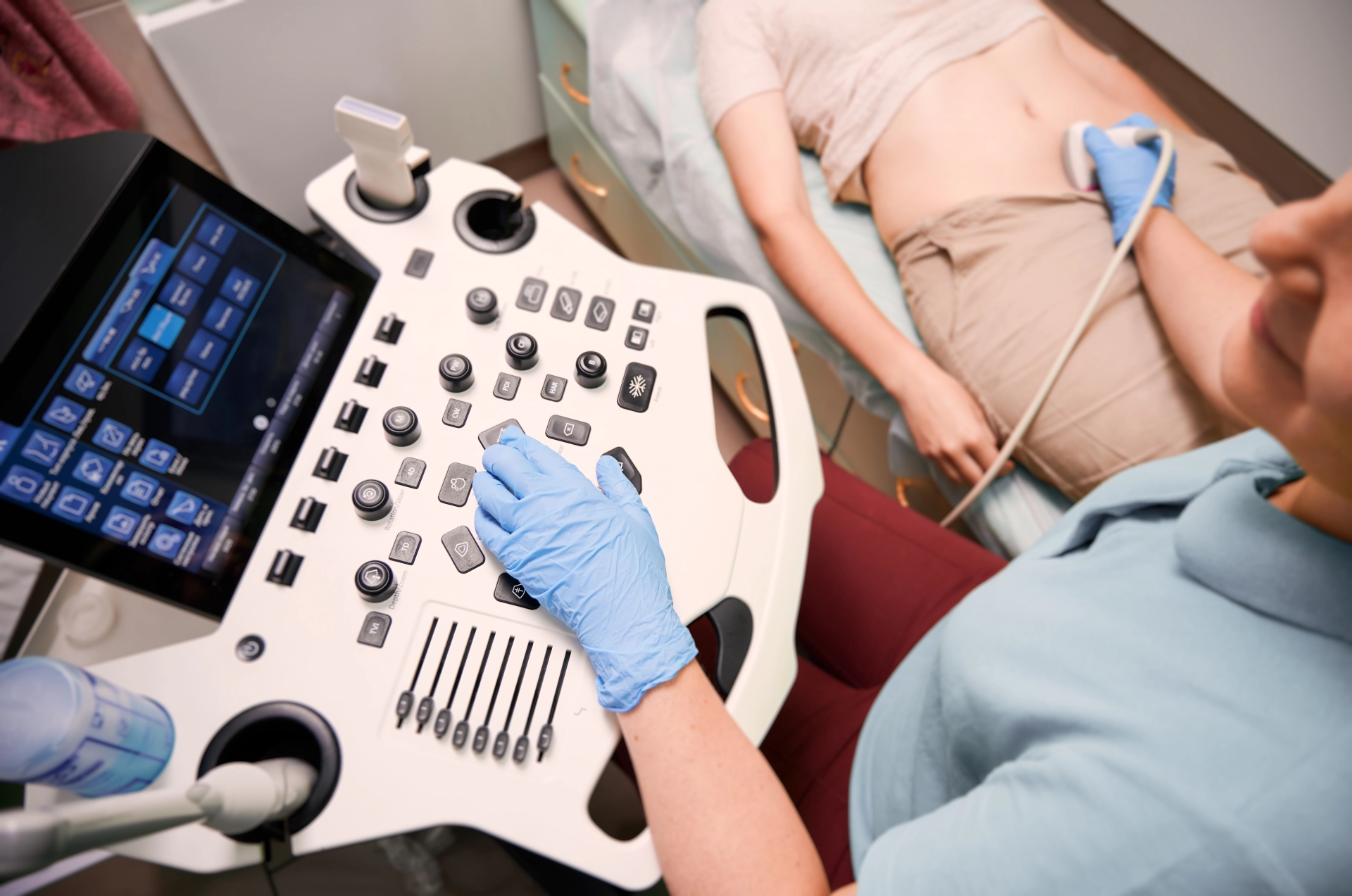
• Breast ultrasound, especially for dense breast tissue
• MRI for high-risk individuals